VASCULAR.EXPERT
mini-invasives
technics
Marc FITOUSSI M.D
Vascular Surgeon.
18-22 Queen Anne Street
W1G 8HU London
+44 20 7034 3326
VASCULAR.EXPERT

Marc FITOUSSI M.D
Vascular Surgeon.
18-22 Queen Anne Street
W1G 8HU London
+44 20 7034 3326


SURGERY : ENDARTERIECTOMY
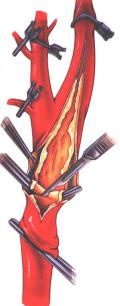


The most common operation is called carotid endarterectomy:
The skin incision, 10 to 15 cm, is located on the lateral face of the neck.
Clamping test verifying the tolerance of the brain to the interruption of carotid arterial flow. If the tolerance is bad the surgeon sets up a temporary shunt.
Arteriotomy: carotid opening
Endarterectomy atherosclerotic plaque: involves removing the atheromatous plaque that obstructs it by cleaving the wall of the artery.
The carotid artery is left in place, but cleaned.
The artery is then closed by a suture either direct or with a patch (piece of prosthesis sewn to the artery so as to increase its diameter)
Unclamping.
The incision is closed by resorbable wire on an aspirating drain.
Exit the following day under platelet anti-aggregating treatment.
Anesthesia is loco-regional, purely cervical.
There is no general anesthesia for 2 reasons:
- there are no surgical contraindications related to old age
- Awakening makes it possible to control the intraoperative cerebral perfusion. The hand of the patient opposed to the carotid artery operated during carotid clamping is shaken. In case of neurological deficit, the surgeon sets up a carotid shunt (external bypass of the circulation) removed at unclamping.
The postoperative recommendations are:
The scar: the suture is made carefully and meticulously and includes several plans, with resorbable son.
- During the weeks or months that follow, there is a more or less important inflammatory reaction (scar red and raised).
- soften your scar a month after the operation, massaging it firmly, between thumb and forefinger, with a simple moisturizer.
- then the scar flattens and fades.
- The final result can only be judged after 6 to 12 months. Only a fine line persists.
The solar exposure of the scar: to avoid especially the first year. put a sticky bandage or a full screen ointment).
Edema (swelling) is usual, and transient. The scar, a little embossed initially, will flatten towards the first month.
Hematomas and bruises: The blues can appear at a distance from the scar and will disappear in 2 to 3 weeks. The blue will first become yellow before disappearing
The showers
Avoid wetting the scar during the first week postoperatively.
If you accidentally wet your dressing, remove it and leave the scar in the air.
After the 2nd week, clean the scar with soap and water, then dry well,
Food, Drinks: Regular Meal, No Absorption
Postoperative treatment: follow the prescriptions, including Aspirin or Plavix
the postoperative consultation towards the first week
POSSIBLE INCIDENTS AND ACCIDENTS DURING OR AFTER INTERVENTION?
In spite of the care taken, it can happen during the intervention, incidents or accidents which are for the most part immediately identified and treated. It can be:
- Peripheral nerve lesions:
In the majority of cases, it is a nerve contusion responsible for transient disorders, regressive in a few weeks:
- The involvement of the cervical sensory nerves is frequent and results in anesthesia of the jaw and earlobe.
- Achievement of the chin branch of the facial nerve causes asymmetry of the face with falling of the labial commissure.
- Lesions of the laryngeal nerves are responsible for voice disorders and require specialized advice (ENT).
- The involvement of the twelfth cranial pair causes paralysis of half of the tongue and soft palate with discomfort to chewing and swallowing.
- Anesthesia accidents are exceptional. Specific information will be provided during the Preoperative Anesthesia consultation.
- compressive cervical hematoma favored by the use of anticoagulants and frequent attacks of arterial hypertension. It results in painful swelling of the neck and difficulty breathing. If it is important, it may require surgical reoperation.
- cerebrovascular accident, which is related to poor tolerance of the brain to abrupt cessation of blood flow or to cerebral emboli during arterial dissection or during the restoration of circulation. It can be a limited accident, quickly regressive or a definite accident. The neurological risk is currently less than 3% in specialized teams.

VASCULAR.EXPERT
mini-invasives technics
18-22 Queen Anne Street W1G 8HU London
+44 20 7034 3326