VASCULAR.EXPERT
mini-invasives
technics
Marc FITOUSSI M.D
Vascular Surgeon.
18-22 Queen Anne Street
W1G 8HU London
+44 20 7034 3326
VASCULAR.EXPERT

Marc FITOUSSI M.D
Vascular Surgeon.
18-22 Queen Anne Street
W1G 8HU London
+44 20 7034 3326
AORTIC ANEURYSM 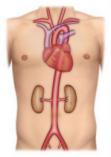
SURGERY
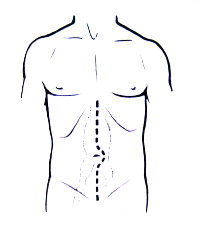
median abdominal scar
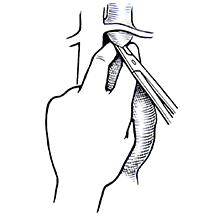
clamping
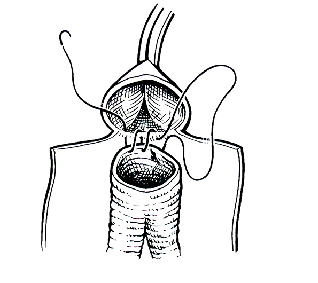
anastomosis
The procedure is performed under general anesthesia. The basic principle of this surgery consists in excluding the aneurysmal pouch (aneurysmal dilatation) from the bloodstream.
The classical treatement or the “flattening – graft” technique, dates from the 60s. It consists in opening the abdomen and implementing a tubular or bifurcated prosthesis made out of polyester (Dacron) at the exact spot of the aneurysm. This prosthetic bypass can be extended to the iliac or femoral arteries, depending on the spreading of the aneurysm. This procedure requires for the patient to be generally in good health and free from any severe cardiac pathologies. The total duration of the hospitalization varies from 8 to 15 days, including a minimum of 24 hours in Intensive Care.
Results
Evidence shows the efficacy of the classic surgery is good. Some problems may arise such as : a weakness of the abdominal wall (eventration), sexual disorders (retrograde ejaculation) and an increase in the chances of aneurysm related pathologies. That is why a frequent monitoring of the situation is required.
What sort of risks can be encountered during the procedure ?
Despite all the care given, incidents during the surgery can happen and are for most identified and taken care of. Such incidents may be :
-Hemorrhages : they usually occur within the first 48 hours, might require a transfusion and a surgical re-intervention.
-Wounding of the nearby vessels (inferior vena cava, iliac), that can lead to hemorrhages. This might require blood transfusions.
-The surgical conversion (classical procedure) in case of a STENT (0-15%), is proposed, either when it is impossible to install the STENT, or in case of an arterial rupture. This procedure becomes rarer as the available tools and standards improve.
-Anesthesia accidents : they are extremely rare. Detailed and specific explications will be delivered to you during the pre-operatory consultation.
What are the post-surgery complications that may arise ?
-Acute ischemia and embolism in consequence to the obstruction from the bypass or the mobilizing of blood clots located in the aneurysmal pouch. In extreme circumstances, this could lead to an amputation of part or all of the lower limbs.
-Acute renal insufficiency (renal failure), most often the consequence of multiple complications (hemorrhages, ischemia) and might require, most often temporarily, to be put under dialysis (artificial kidneys). Sometimes, this is an aggravation of a preexisting kidney insufficiency.
-Acute respiratory failure, related to a previous lung disease (chronic bronchitis) or due to an infectious disease (pneumonia, secondary bronchial infection). This can extend the time under artificial respiration and therefore the time in ICU.
-Intestinal infarction, most often localized at the end of the left colon, which is supplied in blood by the inferior mesenteric artery. The chances of this happening is minimized by a thorough surgical tactic.
-Cardiac complications, topped by the risk of a myocardial infarction. These complications justify the need for a pre-surgery check-up (Doppler, scintigraphy, coronarography) looking for a pathology of the coronary arteries, which must be treated before aortic surgery.
-Phlebitis and pulmonary embolism : the risks are slim, and prevented by the prescription of anticoagulants (blood thinner).
-The global mortality rate ranges from 3% to 7% when it comes to the classic surgery, according to international papers.

VASCULAR.EXPERT
mini-invasives technics
18-22 Queen Anne Street W1G 8HU London
+44 20 7034 3326